Retinal Artery Occlusion
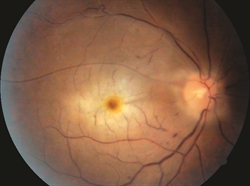
CRAO ©American Society of Retina Specialists
Types of Retinal Artery Occlusion
There are two main categories of arterial occlusion: branch retinal artery occlusion (BRAO) and central retinal artery occlusion (CRAO). BRAO is occlusion of a segment of the retinal arterial system, while CRAO is occlusion of the entire retinal arterial system. The location and degree of vision loss experienced directly correlates to the location and size of the vascular blockage.
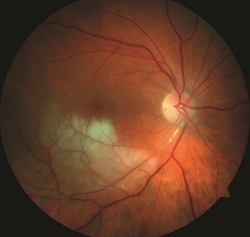
BRAO ©American Society of Retina Specialists
Risk Factors & Symptoms
Risk factors for retinal artery occlusions include advanced age, carotid artery disease, atherosclerosis, valvular heart disease, diabetes, high blood pressure, giant cell arteritis, and blood clotting disorders.
Treatments
The most important aspect of treatment is initiating an emergent stroke work up to identify additional systemic findings associated with risk of stroke.
Retinal arterial occlusion requires immediate, emergent stroke work up in an Emergency Room/Hospital setting as up to 24% of patients presenting with an acute RAO already have concurrent stroke findings on brain MRI. Stroke risk is highest the first 7 days after RAO onset but remains elevated for up to 30 days. In patients over 60, giant cell arteritis, a systemic inflammatory condition must be ruled out as well. Treatment of risk factors to reduce the risk of recurrent RAO is typically coordinated with a neurologist.
Unfortunately, most patients with RAO suffer permanent partial or complete vision loss due to a lack of oxygen delivery and damage to the underlying retinal tissue. Retinal tissue sustains permanent damage after 90 minutes without oxygen delivery. To this day, there has not been a proven method to consistently and reliably reverse vision loss after RAO.
Weeks to months after onset of RAO, patients can develop a secondary complication of abnormal blood vessels growing on either the retina or iris called neovascularization. These abnormal blood vessels can cause bleeding, retinal detachments, and glaucoma in the worse case scenario and may require laser treatment or injections of medication into the eye. These treatments are not a “cure” but can manage the disease quite effectively in many situations.
Retinal Artery Occlusions Fact Sheets
Download the following documents to learn more about age-related macular degeneration.
Conclusion
In summary, RAOs occur when flow of oxygenated blood to the retinal tissue is obstructed and can cause rapid and permanent vision loss. Patients with RAO are at risk for developing cerebrovascular stroke and require immediate stroke evaluation.
Emergent Stoke Evaluation – FOR PROVIDERS
For providers, if you have diagnosed a patient with acute retinal ischemia, either a Branch Retinal Artery Occlusion (BRAO), a Central Retinal Artery Occlusion (CRAO), or a temporary loss of vision that might be related to a blocked artery, called Transient Monocular Vision Loss (TMVL) please read.
A Retinal Artery Occlusion is serious as a stroke in the brain, and your patient could be at risk of a major stroke. This condition requires emergent stroke risk evaluation, including carotid ultrasound, echocardiogram and neuroimaging (preferably diffusion-weighted MRI, also called DWI-MRI*). CRAO and other types of sudden monocular vision loss—such as BRAO or retinal transient ischemic attack—greatly increase the risk of silent brain infarctions. Since these 3 conditions significantly increase the risk for subsequent clinical strokes, we advise you send your patient for an urgent and thorough evaluation at a Level 1 Comprehensive Stroke Center, within 24 hours if possible. Follow the steps below to refer a patient to a Level 1 Comprehensive Stroke Center:
- Finish and print your chart note detailing the concern for stroke for your patient to take with them to the ER.
- Print and fill out the stroke evaluation form (change to your office information).
- Instruct your patient to go to a Level 1 Comprehensive Stroke Center ASAP (within latest 24 hours) – Colorado stroke centers are listed on the back of the form, organized by geographic location.
- Call the emergent line at the stroke center the patient is headed to and provide them with your patients’ full name, date of birth, ocular and medical symptoms, and potential diagnosis.
- Send/fax any supporting documents/imaging you have over to the stroke center.
Schedule a Retinal Artery Occlusion Consultation with Colorado Retina Associates
As the premier retina practice of the Rocky Mountains, Colorado Retina Associates provides advanced diagnostic care and treatment for Retinal Artery Occlusion. Schedule a consultation today with one of our retina specialists in the Denver, Boulder, Aurora, and Lakewood areas.

