Flashes & Floaters
Flashes and/or floaters can be a startling occurrence. Floaters typically start as sudden, painless opacities like thousands of little specks (sometimes described as pepper or dust by the patient) or larger stringy opacities (sometimes described as cobwebs or hair). Flashing lights may accompany these new floaters as bright arcs of light in the far peripheral or side vision. Flashes and floaters may alternatively have a more gradual onset where the floaters slowly increase in number and the flashing lights have a more shimmering or mirage-like quality.
Causes & Symptoms
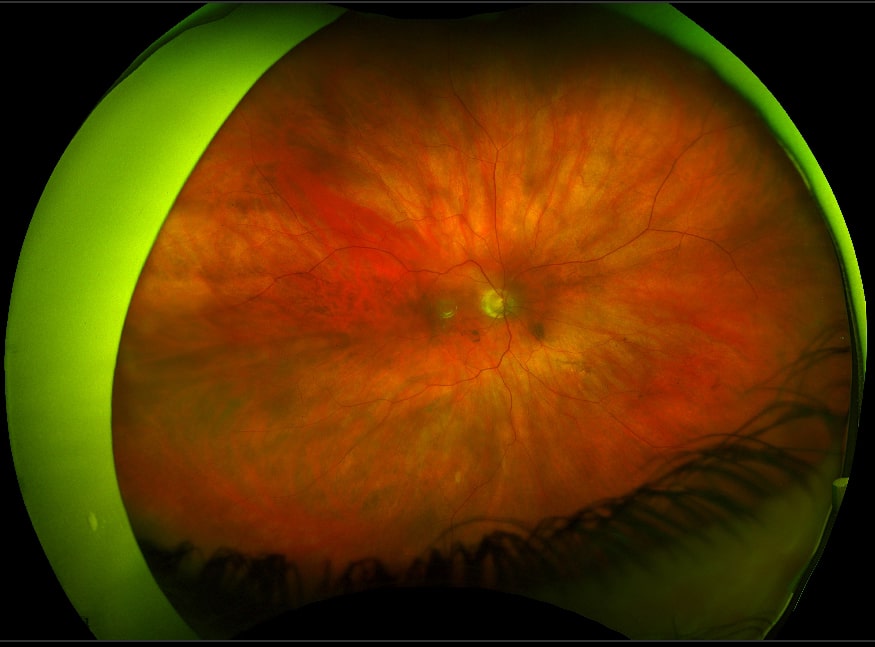
Floaters may be a single large opacity as in the Weiss ring shown above.
The sudden onset of floaters and flashing lights is usually associated with posterior vitreous detachment, particularly when they occur in a patient’s 50’s or 60’s. The vitreous is the gelatinous structure that fills the back of the eye, having served its role primarily in the development of the eye. As the gel breaks down it liquifies and finally collapses, pulling itself free from the retina. Only the posterior aspect of the gel separates from the retina, hence the term posterior vitreous detachment (PVD). Once floating freely, opacities in the vitreous and along its posterior face (the posterior hyaloid or vitreous cortex) are more apparent in the vision. The arcs of flashing lights in the peripheral vision are caused by gentle traction at the leading edge of the vitreous separation from the retina.
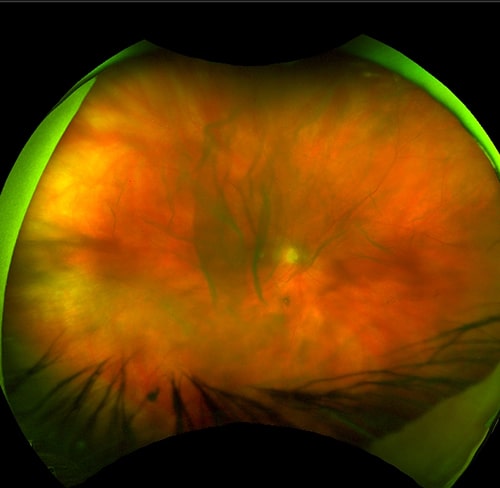
Or floaters may be more dense and widely distributed throughout the gel.
Most of the time, PVD formation is a benign process that does not threaten the vision. However, sometimes it can pull on the retina, causing a retinal tear. If not treated in time, a retinal tear can lead to a retinal detachment. The detached retina causes a shadow to occur in the vision which can spread throughout the vision if not treated. Because there is no way to tell if new floaters or flashing lights represent a simple PVD, or a tear or detachment, it is recommended to seek care promptly. Please call our office if you are concerned you are having new floaters or flashing lights.
A retinal tear can lead to a retinal detachment. Floaters are often the first warning sign of a problem.

Hello world!
Another cause of sudden onset, painless floaters, is bleeding in the vitreous. Blood in the eye can form long, stringy opacities as the red blood cells may be trapped in one of the vitreous gel’s many cisterns. The red blood cells can also be dispersed like a drop of ink in water, resulting in thousands of little specks and a diffuse haze. In patients with diabetic retinopathy, bleeding in the eye may represent the development of proliferative diabetic retinopathy, a condition where abnormal blood vessels grow along the surface of the retina and the vitreous gel. In patients with risk factors for atherosclerosis (high blood pressure, diabetes, high cholesterol, smoking, family history, sleep apnea, age, etc), bleeding may occur from a blockage of a retinal vein. Bleeding in the eye may also be associated with trauma, diabetes, hypertension, violent valsalva (bearing down), and congenital vascular malformations. Finally, a PVD with or without a tear or detachment can cause bleeding in the eye.
A more gradual onset of floaters and/or shimmering flashing lights throughout the central vision can be a symptom of inflammation in the eye. Inflammation in the eye may be caused by an autoimmune condition, either isolated to the eye or in association with systemic disease. An infection is another common cause of inflammation in the eye. The severity can range from a mild viral infection or represent a serious life threatening bacterial illness. In older patients, the development of floaters can occasionally be caused by cancer.
Treatment
In most cases of degenerative floaters (those associated with the normal breakdown process of the gel), the symptoms are mild and often completely overlooked by the brain after a period of adaptation. If the opacities interfere with a patient’s ability to function, surgery is an option. Certain patients with a single large opacity may find some improvement with a laser treatment. In patients with floaters secondary to an underlying condition, identification and treatment of that condition is paramount to preserving vision.
Surgery
In the past, vitrectomy surgery was performed with large incisions, instrumentation and sutures; a high rate of complications and long recovery period limited its utility to only the most affected patients. Now surgery can be performed with a minimally invasive sutureless system, employing 25 or 27 gauge instruments on an outpatient basis. Though recovery is much faster (typically a few days to a week), there is still a small risk of vision threatening complications. For this reason, it is important to have a careful conversation with your surgeon before considering vitrectomy. Your surgeon may also recommend a period of observation and reflection on the impact of the floaters on your quality of life prior to agreeing to surgery.
Post-Surgery
The recovery from 25 or 27 gauge surgery is generally quick and painless. The vision will usually be blurry for the first few days but then return to normal levels within a week, with an often complete resolution of symptoms. Eye drops will be given for 10-14 days and light activity will be advised for 1-2 weeks. Non-physical work can often be resumed within a few days of surgery.
The general risks of surgery include bleeding, infection, and retinal detachment. Macular edema, macular pucker, and reactions to anesthesia are also possible. While these risks are small, they can lead to blindness and so a careful consideration of the risks versus benefits of the surgery is crucial. It is also worth remembering that cataract progression will accelerate after vitrectomy, thus requiring cataract surgery sooner that would otherwise be necessary. For patients that have already had cataract surgery, vitrectomy for floaters will not affect the lens implant. Your glasses prescription may change slightly as a result of surgery, though usually this is more a function of accelerated cataract progression if it occurs.
Conclusion
Floaters are a common symptom representing a wide variety of underlying conditions from benign to vision threatening. When occurring acutely, accompanied by flashing lights, or associated with a decrease in vision, they often warrant urgent evaluation. If floaters become a persisting problem and limit a patient’s quality of life and ability to function, they can often be treated effectively with minimally invasive surgery.
Need more information?
Schedule a Flashes & Floaters Consultation with Colorado Retina Associates
As the premier retina practice of the Rocky Mountains, Colorado Retina Associates provides advanced diagnostic care and treatment for Flashes & Floaters. Schedule a consultation today with one of our retina specialists in the Denver, Boulder, Aurora, and Lakewood areas.

